Pancreatic beta-cell dysfunction causes diabetes
Published : 17 Sep 2018, 01:08
Updated : 17 Sep 2018, 11:41
Dysfunction of insulin-producing pancreatic cells is the ultimate cause of diabetes.
A new doctoral study introduces a novel model to study the molecular mechanisms behind this dysfunction with the help of pluripotent stem cells and CRISPR-Cas9 gene editing, said a press release issued by University of Helsinki.
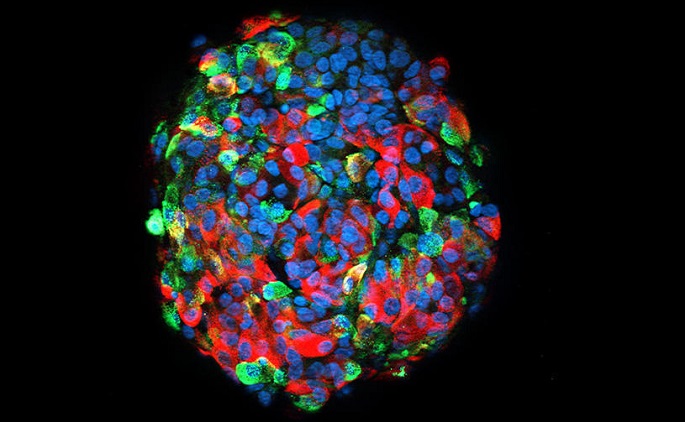
The main cause of all forms of diabetes is pancreatic beta-cell dysfunction. Beta-cells, found in the pancreatic islets, store and release insulin.
Decades of research with animal and cellular models have expanded the knowledge on the molecular mechanisms causing the beta-cells to dysfunction. Diego Balboa’s doctoral research now offers a more precise model that employs human pluripotent stem cells.
“Human pluripotent stem cells constitute a renewable source of beta-cells. Stem cell-derived beta-cells can be generated by directed differentiation and used as a model to study pancreatic beta-cell development and disease in vitro,” Balboa explained.
Compared to the novel method, the traditionally used animal and cellular models have limitations that may significantly affect the way the findings can be translated into new approaches to combat diabetes in humans. For example, rodent pancreatic islet development and physiology differ from that of humans, and rodent and human insulinoma cell lines do not recapitulate faithfully the functionality of adult human beta-cells.
So far the best model has been the cadaveric donor human islets that are scarce, and difficult to manipulate for certain experiments.
Balboa’s research demonstrated the use of human pluripotent stem cells as a tool to investigate monogenic diabetes disease mechanisms. The cells can also be transplanted into immune-compromised mice, generating humanised models where in vivo beta-cell function can be closely evaluated in a systemic context.
“For this purpose, improved human pluripotent stem cell differentiation protocols to the beta-cell lineage were generated utilizing 3D suspension culture approaches,” said Balboa.
In his research, Balboa also established novel CRISPR-Cas9-based gene editing techniques to model monogenic diabetes cases.
“Using these approaches, an activating mutation in STAT3 gene was found to cause neonatal diabetes by inducing pancreas endocrinogenesis prematurely. In a similar way, INS gene mutations causing pro-insulin misfolding were found to impair developing beta-cell proliferation due to increased endoplasmic reticulum stress.”
Diego Balboa Alonso will defend the doctoral dissertation entitled ‘Human Pluripotent Stem Cells and CRISPR-Cas9 Genome Editing to Model Diabetes’ at the Faculty of Medicine, University of Helsinki, on 21 September.